Letícia Soares stepped off the plane in Brazil feeling traumatized and vulnerable. It was 2021 and she was returning home from Canada, where the final year of her postdoc in disease ecology had been marred by long COVID. The condition left her with searing migraines, intense fatigue, body aches and a variety of other ailments that came and went unpredictably, but never improved. Soares decided to return home where she felt she would have better access to medical support if she were disabled and unemployed.
Having encountered dismissive physicians in Canada, she hoped she would be better supported at home. But her arrival brought fresh disappointment. More than a year into the COVID-19 pandemic, Soares’ physicians, friends and family in Brazil had still not heard of long COVID. “People asked me whether long COVID is an illness of the global north,” says Soares, who now works from Salvador, Brazil, at the Patient-Led Research Collaborative, an international advocacy and research organization focused on long COVID and associated conditions. “They had never heard of it here.”
By some estimates, more than four million people in Brazil have long COVID. Yet researchers say the reaction that Soares encountered is common in many low- and middle-income countries (LMICs). Much of the world’s research on long COVID is conducted in wealthy regions, and data on the prevalence or severity of the condition in other locales are more limited (see ‘Dearth of research’). “The main story about long COVID in low- and middle-income countries is that there are relatively few studies,” says Theo Vos, an epidemiologist at the Institute for Health Metrics and Evaluation in Seattle, Washington. “But wherever people have looked at it, they find it.”
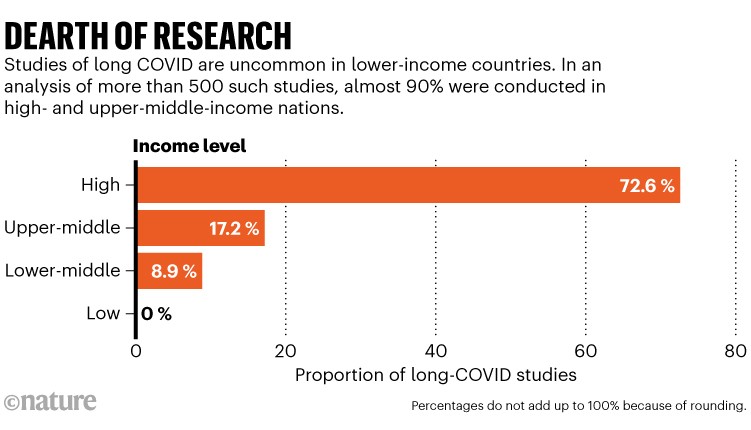
Source: J. V. A. Franco et al. Int. J. Environ. Res. Public Health 19, 9915 (2022)
Evidence so far suggests that the prevalence of long COVID in LMICs could be similar to that of wealthier countries — although, in both settings, the numbers vary a lot. One review1 found that between 8% and 41% of people who had a SARS-CoV-2 infection but weren’t hospitalized had symptoms. But a dearth of research on the condition in less-wealthy countries creates a double curse. An absence of information about prevalence and risk factors leaves advocates hamstrung: few physicians acknowledge that long COVID exists. The lack of data also hampers efforts to search for the mechanisms of the condition and tailor treatments. “You need data for action,” says Waasila Jassat, a public-health specialist at Genesis Analytics, a consultancy firm in Johannesburg, South Africa. “You need evidence to advocate for services, and you cannot just use data from other countries.”
Unknown prevalence
Table of Contents
Long COVID is a complex condition brought on by infection with SARS-CoV-2. It has been linked to more than 200 symptoms, from brain fog or fatigue that makes it difficult to work, to debilitating pain and muscle weakness. The severity of the condition can vary, and for many people symptoms come and go; there are days when they can function as they did before or nearly so, only to find that their condition comes roaring back a day later. By some definitions, the condition includes any symptoms that appear or persist for more than three months after the initial infection.

Long COVID research risks losing momentum — we need a moonshot
All of this makes the burden of long COVID difficult to measure, even in resource-rich countries. It’s even harder to compare across studies, because different research groups might focus on various definitions and symptoms, or survey different groups of people.
LMICs — a heterogeneous collection of more than 130 nations — face even more challenges. Many have been undermined economically by a legacy of colonialism and exploitation. Health-care systems vary widely among these countries, but resources are strained in many of them relative to wealthier countries. It is already difficult to find resources for research, and that’s compounded by the lack of centralized health data, says Jassat. In Brazil, for example, more than one-third of all workers are informally employed, meaning that there is no systematic way to track how many days of work people miss due to illness.
“People are quietly dropping out of society,” says Emma-Louise Aveling, a global public-health researcher at the Harvard T.H. Chan School of Public Health in Boston, Massachusetts, who has interviewed health-care workers and people with long COVID in Brazil for her research.
Scientists have been trying to pin down the number of people with the condition. Worried that the burgeoning COVID-19 pandemic could worsen or lead to new cases of chronic illnesses, cardiologist Nizal Sarrafzadegan at the Isfahan University of Medical Sciences in Iran launched a long-term study in March 2020. Her team found that 60% of individuals who were hospitalized with COVID-19 in Iran had symptoms a year after their infection2.
In South Africa, Jassat and her colleagues followed 3,700 people for 6 months in a study3 of COVID-19 outcomes and found that 39% still had at least one symptom 6 months after their initial infection. People who were hospitalized owing to COVID-19 were more likely to be affected than those who were not: 46.7% versus 18.5%.
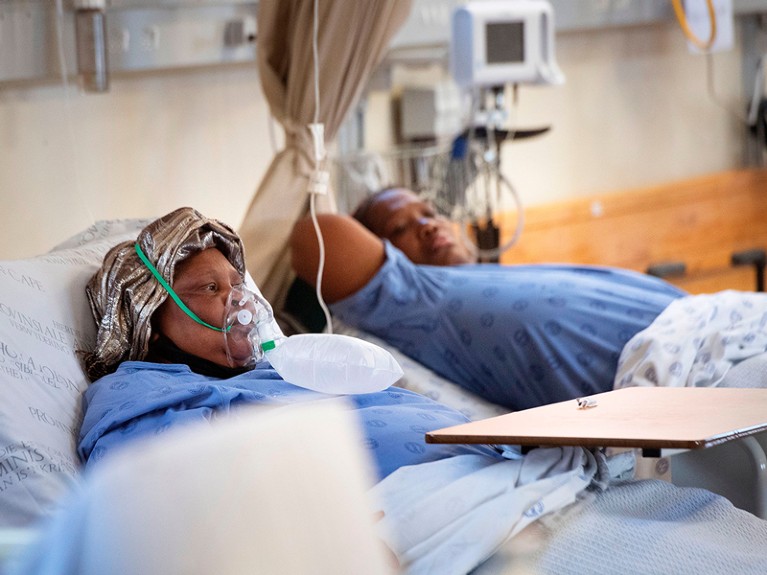
People hospitalized with COVID-19 are more likely to be affected by long COVID.Credit: Rodger Bosch/AFP/Getty
In a 2020 study, geriatricians Murilo Dias and Márlon Aliberti at the University of São Paulo, Brazil, and their colleagues found that one in three people admitted for COVID-19 to a hospital in São Paulo still had at least one symptom a year after they were discharged4. “That’s a huge problem for the health system,” says Aliberti.
Even so, that problem does not include cases of long COVID that arise after mild SARS-CoV-2 infection. Soares says that most long-COVID studies in Brazil do not address this gap, and it can be particularly hard to do so when few physicians are aware of the condition, how to diagnose it or who might be at particular risk.
Another reason to study long COVID in different contexts is that the condition might manifest differently from place to place. Many researchers suspect that there are multiple mechanisms underlying long COVID. The risk of the condition might be influenced by genetic and environmental factors, says Olufemi Erinoso, a public-health researcher at the University of Nevada in Reno, who has studied long COVID in Lagos, Nigeria. “We need to have a global approach to the disease to understand how genetics might affect the outcomes.”
Diverse data
To really grasp the mechanism of long COVID, researchers need study participants with diverse genetic backgrounds so that they can work out which cellular pathways are involved and how they might vary in different people. And the more researchers know about those pathways, the more potential targets they’ll have for medicines to treat long COVID. “Not being able to approach the disease in a global, concerted effort is a major impediment to a better understanding and a better therapy for everyone,” says Akiko Iwasaki, an immunologist at Yale University in New Haven, Connecticut.

Long COVID: answers emerge on how many people get better
One trend that looks to be consistent worldwide is that the number of people who develop long COVID seems to be tapering off with the SARS-CoV-2 variants over the past two years. In South Africa, Jassat and her colleagues found a lower incidence of long COVID among those infected with the Omicron variant, compared with the Beta or Delta variants of the virus3. UK researchers similarly found that Omicron infections were less likely than were Delta infections to lead to long COVID5. The world has long since moved on from Omicron, but researchers suspect that growing levels of immunity — from vaccination and infection — could also be reducing the number of people at risk of developing long COVID across the globe, says paediatrician Daniel Munblit at Imperial College London, who has studied long COVID in children in Moscow.
This is good news, with one small downside: new studies of long COVID could struggle to recruit participants. This year, Tariro Makadzange, executive director of the research organization Charles River Medical Group in Harare, and her colleagues had trouble including the condition in a study because they found so few fresh cases.
Tailoring treatment
In the United States and Europe, large-scale efforts have begun the search for long-COVID treatments. The US National Institutes of Health is running the US$1.15-billion Researching COVID to Enhance Recovery (RECOVER) programme, some of which is directed at finding long-COVID therapies. In the United Kingdom, a consortium of 30 hospitals and universities is also looking for treatments under the STIMULATE-ICP programme.
But whether any resulting treatments could transfer to lower-income settings is an open question, says infectious-disease specialist Luis Felipe Reyes at the University of La Sabana in Bogotá. He predicts a re-run of the inequalities that plagued the distribution of COVID-19 vaccines. Wealthier countries hoarded doses and some types, such as the mRNA vaccines, were particularly difficult for many lower-income countries to use because they were expensive to produce and difficult to transport at the low temperatures they require.

Are repeat COVID infections dangerous? What the science says
“The rich countries are finding the treatments for these problems, but those solutions might not be transferable,” Reyes says.
For now, treatments for long COVID often involve careful rehabilitation and, ideally, a collaborative team of specialists in different fields. Such intensive monitoring and care is difficult even for wealthy nations, let alone for countries with more strained health-care systems, says Kimberly Konono, a vaccine specialist at Charles River Medical Group. But even with limited resources, some LMICs have options that are not available in wealthier nations. For example, the public health-care system in Brazil includes a network of community health workers who are embedded in neighbourhoods and often know the occupants well. This network could be used to improve awareness, diagnosis and treatment of long COVID in these regions, says Aveling.
But even that approach relies on health-care systems taking the condition seriously, which hasn’t always happened with some other post-viral illnesses. Similar conditions can follow after other viral infections, including some tropical diseases. These have long been neglected, says anthropologist Jean Segata at the Federal University of Rio Grande do Sul in Porto Alegre, Brazil, particularly when they affect marginalized communities. “Often, these patients complain that they are not taken seriously by doctors, who tell them it’s nothing and that it will pass soon,” he says. “The lack of recognition for their suffering becomes an additional source of frustration and distress for long-COVID patients in impoverished countries.”
Soares, who has been working with Aveling and others to characterize the impact of long COVID in Brazil, can see the effect of this: long COVID and other post-viral illnesses are effectively invisible. “We need to show with data that people are going through these symptoms and the challenge that needs to be addressed,” Soares says. Then she sighs. “I wish that we didn’t have to.”
